Consider the Pros and Cons of a Surgical Vs. Surgery-free Procedure
Seeing a Meniscus tear on your MRI doesn’t necessarily mean you need to have surgery. If you’re experiencing low back pain, knee pain, or any other joint/orthopedic pain, consider the pros and cons of a surgical vs. surgery-free procedure.
What is a Meniscus Tear?
In your body, you have a total of 4 menisci (the plural of meniscus), two on each of your knees. Each one is white, rubbery, shaped like a “C” and acts as a shock absorber for your knees. They protect the other parts of your knee from the impact and stress that everyday use can cause [1].
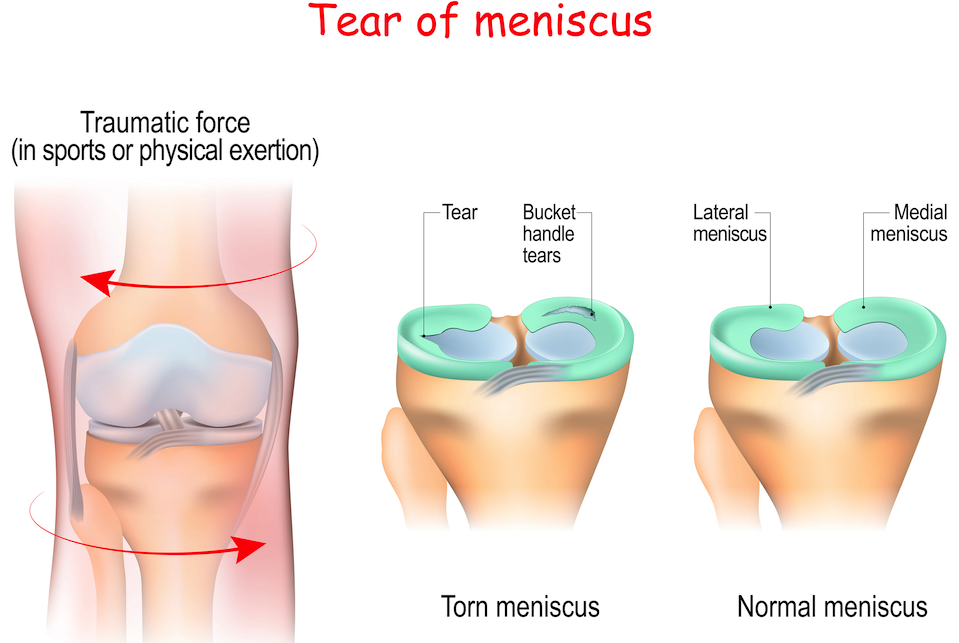
A meniscus tear occurs when this C-shaped structure is damaged. While some people experience traumatic meniscus tears (caused by rotating, twisting, or deep bending of the knee), many people simply experience meniscus tears due to the gradual wear-and-tear that occurs in everyday life [1]. Meniscus tears are so common that they could be considered a natural part of aging [2]. A majority of people over the age of 35 would have an MRI come back showing a Meniscus Tear [1].
Does this Mean You Need Surgery?
Some people believe that if you see a tear on an MRI, then you should get surgery. This is actually not true. What type of treatment you should get depends a lot on what kind of tear you have and your symptoms.
Meniscus injuries, or problems in your knee’s cushions/shock absorbers, are extremely common. There are many different types of meniscus tears and sometimes these can cause pain and/or mechanical symptoms in the knee, such as catching or locking. Meniscus tears can be caused abruptly by an injury or can be degenerative, meaning they fray with wear and tear over time. It is important to know that just because a meniscus tear is present on an imaging study, depending on the type of tear, it may or may not be causing pain. As much as 61% of people with meniscus tears experience no symptoms [3]. In fact, studies have shown that when looking at elderly and middle-aged patients, those who weren’t experiencing knee pain were equally likely to have or not have a meniscus tear [4].
Before deciding on a course of action, an orthopedic doctor needs to look at how the injury is affecting you specifically.
To Surgery or Not to Surgery
If you’re experiencing low back pain, knee pain, or any other joint/orthopedic pain, consider the pros and cons of a surgical vs. surgery-free procedure. Before you commit to invasive orthopedic surgery, please watch Dr. booth in this under 4-minute video.
What to Expect with a Meniscus Surgery
There are two kinds of meniscus surgery: A Meniscus Repair and a Full or Partial Meniscectomy. The first is exactly as it sounds: a surgery to repair the tear in the meniscus and allow it to heal. This seems straightforward, but of the more than 700,000 Meniscus surgeries that occur every year, only about 4% are true repairs [5]. These repairs are only done for specific types of tears–mainly those that include a part of the meniscus flipping over inside the knee. If left alone these tears could cause additional complications [6].
The remaining 94% of surgeries are full or partial Meniscectomies. This is a surgery that removes torn fragments or trims the meniscus back to try and reduce the experienced symptoms. Unfortunately, these surgeries have been shown to be no more effective than just physical therapy [7].
Additionally, these surgeries can lead to rapid deterioration of the knee [3]. One study found that 60% of patients who had a Meniscectomy developed arthritis within a few years [5]. The cause seems to be an increase in the amount of force walking places on the knees. With the Meniscus removed or reduced, there is more stress on the knee which will lead to an increased speed of degeneration [5].
Alternatives to Surgery
Aside from surgery, there are several other options for treating a meniscus tear. These treatments accomplish different things and can work for different kinds of pain or tears:
- Natural Remedies
If you are experiencing knee pain and a meniscus tear is suspected or confirmed, one of the first steps should be the natural ones. With rest, physical therapy, and some good nutritional support, many meniscus tears heal in 4-6 weeks. Exercises that focus on range of motion and strengthening the surrounding muscles can help also. - Steroid Injections
Steroid injections are often recommended by primary care physicians after physical therapy. Our Regenexx doctors believe that steroid injections should be avoided. These injections work by reducing inflammation, which can reduce the symptoms of a meniscus tear, but do little to treat the problem. Steroids also come with negative side effects like inhibiting healing or damaging the cartilage in your joints. - Hyaluronic Acid
This is a part of the lubricating fluid that keeps the parts of your joints moving smoothly. Similar to Steroid injections, an injection of hyaluronic acid works as a source of temporary pain relief, but not an actual treatment. - Platelet Rich Plasma (PRP)
PRP uses growth factors from your own body to help the meniscus to repair itself. Platelet injections have a stimulating effect on the repair cells/your own stem cells within the targeted area, making those cells work harder to perform their natural job of healing the body. This treatment has been found to help heal meniscus tears as well as mild to moderate arthritis. - Bone Marrow Concentrate (BMC)
Regenexx’s patented SD procedure uses Bone Marrow Concentrate containing your own live stem cells. These are the same stem cells that PRP makes work even harder. These repair cells from your own body live inside all of us in various tissues, poised to leap into action to repair damage as it occurs.As we age or have big injuries, we may not be able to recruit enough of these cells to the site to fully repair the area. The Regenexx-SD Procedure helps overcome this problem by harvesting bone marrow from an area of the back of the hip that contains a dense population of these important cells and then concentrating those cells before precisely injecting them into the injured area using advanced imaging guidance. The goal of the procedure is to reduce pain and improve function by promoting the body’s own ability to heal naturally.
BMC via the Regenexx SD procedure has been effective for treating more severe meniscus tears and moderate to severe arthritis. [6]
How Regenexx’s PRP and BMC Procedures are Different
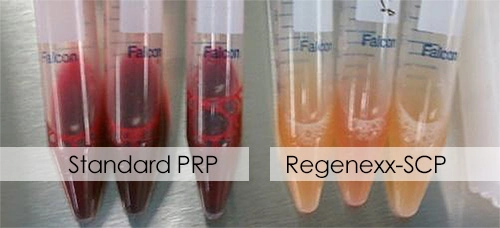
In most clinics that offer PRP therapies, the method of developing PRP involves removing a patient’s blood and running it through a simple bedside centrifuge machine to separate the plasma and concentrate the blood platelets. These devices are not effective at getting rid of unfavorable cells from the resulting mixture, and our lab tests show that white and red blood cells have an inhibiting effect on the same stem cells the platelets are attempting to stimulate.
With a Regenexx procedure, PRP is purer, and more concentrated, because it is produced in a laboratory setting by an experienced technician. Because of its concentration levels of platelets, Regenexx’s Super Concentrated PRP has been shown to deliver up to 10 – 40x times more platelet concentrations than the standard PRP. We have found that better concentrations facilitate better healing [9].
As regenerative medicine has gained popularity over the last two decades, so-called “stem cell therapy clinics” have been popping up all over the country. The treatments offered from these kinds of clinics are often ineffective due to outdated technology, unqualified staff, and/or a lack of testing and research. Since 2005, Regenexx has set the bar and differentiated its BMC procedures from these clinics through several distinct offerings including more advanced technology, treatments, expertise, and research methods.
Regenexx procedures are conducted using high-level imaging guidance to get the PRP and BMC right where it can help the most. Additionally, these treatments have a quicker recovery time. You can be back to your daily routine in 2-5 days, and back to playing sports in 3-6 months, allowing you to get back in the game faster [9].
Only Regenexx Keeps a Patient Outcomes Registry
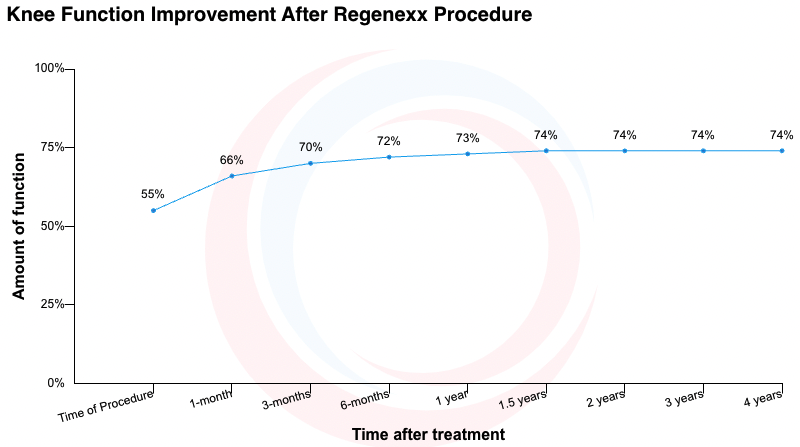
Based on over 12,729 patient procedures tracked, prior to treatment, patients report being limited to an average of 55% of their optimal knee function. Shortly after receiving treatment, they report averages up to 74%. [10]
See more data about how Regenexx procedures have been effective for our patients.